When someone with cirrhosis starts swelling in their belly, it’s not just discomfort - it’s a warning sign. That fluid buildup, called ascites is the abnormal accumulation of fluid in the abdominal cavity, often caused by advanced liver disease. About half of all people with cirrhosis develop ascites within 10 years, and once it shows up, survival drops sharply - only about half live past two years without intervention. The real problem isn’t just the fluid. It’s what’s driving it: high pressure in the liver’s blood vessels and your body holding onto too much salt and water. Managing ascites isn’t about one magic pill. It’s about two things most doctors agree on: sodium restriction and diuretics. But even those basics are now under fire.
Why Salt Matters More Than You Think
Your kidneys normally flush out extra sodium. But when your liver is damaged, your body gets confused. It thinks it’s low on blood volume, even though you’re full of fluid. So it clings to salt like a lifeline. Every extra gram of sodium you eat? Your body holds onto it - and pulls water with it. That’s how ascites grows. The traditional fix? Cut sodium hard. Most guidelines, including those from the American Association for the Study of Liver Diseases (AASLD), say keep it under 2 grams a day. That’s roughly one teaspoon of table salt. Sounds simple, right?
Here’s the catch: most people don’t get their sodium from the salt shaker. About 75% comes from packaged foods - bread, soup, deli meats, canned veggies, even breakfast cereal. Trying to stick to 2 grams means reading every label, cooking everything from scratch, and saying no to almost every restaurant meal. Studies show less than 40% of patients can actually stick to that level. And when they fail, they feel defeated, not disciplined.
Now, here’s where things get controversial. A handful of recent studies, including a 2022 paper in Gut and Liver Journal, found that patients on a moderate sodium diet (5-6.5 grams of salt per day) actually had better outcomes than those on strict restriction. They had less ascites, needed fewer hospital procedures, and didn’t crash their kidney function as often. Why? Because too little sodium might drop your blood pressure too far, making your kidneys shut down even more. That’s when hepatorenal syndrome - a deadly kidney failure linked to liver disease - becomes more likely.
Diuretics: The Medication That Makes You Pee
If salt restriction is the brake, diuretics are the gas pedal. They force your kidneys to dump sodium and water. The first-line drug is spironolactone. It’s a potassium-sparing diuretic that blocks the hormone aldosterone, which is overactive in liver disease. Doctors start with 100 mg daily and increase every three days, up to 400 mg if needed. It works slowly - you might not see results for a full week. But it’s effective. In uncomplicated cases, spironolactone alone helps 80-90% of patients lose fluid.
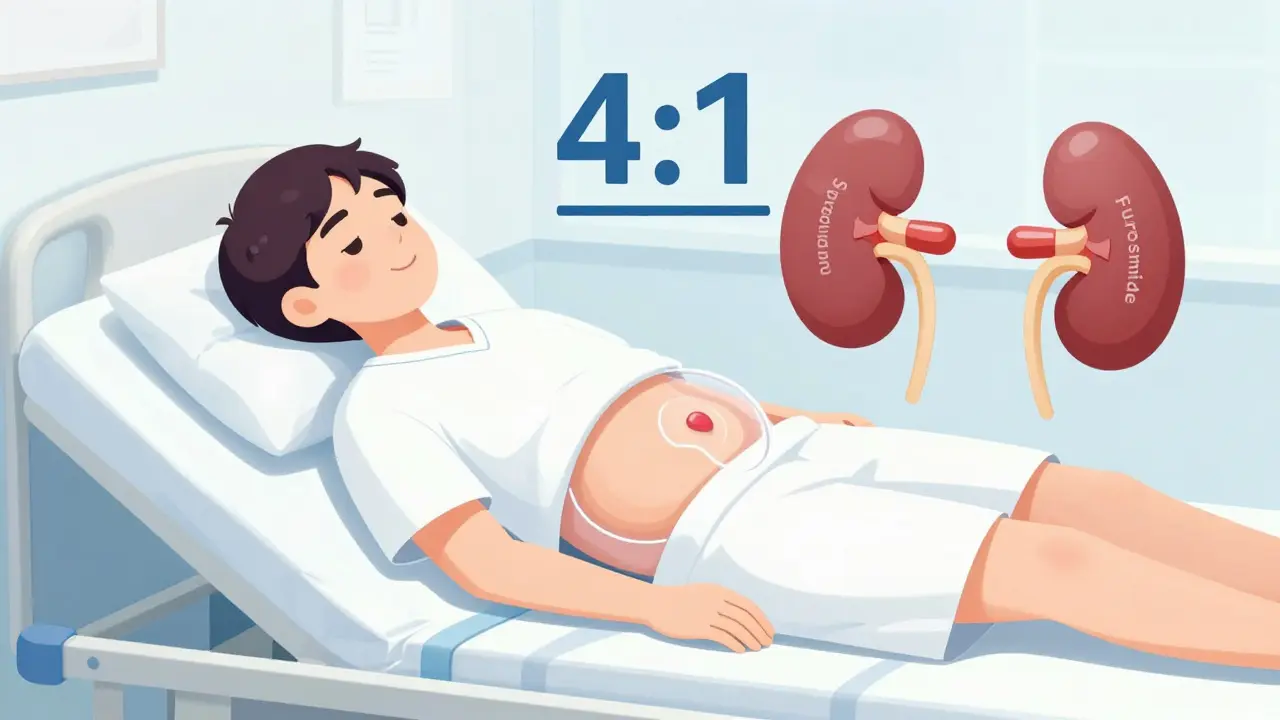
But if that’s not enough? Enter furosemide. This is a loop diuretic, stronger and faster-acting. It’s often added when spironolactone hits its limit. The usual combo is 100 mg spironolactone and 40 mg furosemide. The ratio matters: 4:1 is standard. Too much furosemide without enough spironolactone? You risk low potassium, low blood pressure, and kidney damage. Doses can go up to 160 mg furosemide, but only under close watch.
Goal? Weight loss. Not fat loss. Fluid loss. For patients without leg swelling, aim for no more than 0.5 kg (about 1 pound) per day. If they have swollen legs too, you can go up to 1 kg per day. Go faster than that, and you risk shocking your system. Your kidneys need time to adjust. That’s why doctors check your blood sodium at least twice a week in the first few weeks. A sudden drop in sodium? That’s hyponatremia - a dangerous drop in blood salt levels. It’s common in ascites patients. If your sodium falls below 130, you might need to tweak diuretics or even restrict fluids.
The Hidden Dangers: What You Must Avoid
It’s not just about what you take - it’s about what you don’t. Many common medications make ascites worse. NSAIDs like ibuprofen or naproxen? They reduce blood flow to the kidneys. In someone with cirrhosis, that’s like cutting off a lifeline. Studies show using NSAIDs increases the risk of kidney failure by more than double. Same goes for ACE inhibitors and ARBs - drugs used for high blood pressure. These can drop kidney function fast in cirrhotic patients. One study found they raise the risk of end-stage kidney disease by 2.3 times.
Even over-the-counter supplements can be risky. Herbal remedies like milk thistle or dandelion root? They’re not regulated. Some interfere with liver metabolism or diuretic action. And don’t forget alcohol. Even small amounts accelerate liver damage and worsen fluid retention. There’s no safe level once ascites appears.
When Diuretics Don’t Work: The Refractory Reality
Not everyone responds. About 5-10% of patients develop refractory ascites - fluid that won’t budge, no matter how high the diuretic dose. These patients have a grim prognosis. Half won’t survive past six months. For them, the only reliable option is large-volume paracentesis. That’s a procedure where a needle drains up to 5 liters of fluid at once from the abdomen. It works fast. But it’s not a cure. Fluid comes back, often within weeks.
That’s why albumin is critical. Every liter of fluid removed needs 8 grams of human albumin given intravenously. Why? Because pulling out fluid also pulls out proteins that keep blood pressure stable. Without albumin, you risk a sudden drop in blood pressure - even shock. This procedure requires a hospital visit, trained staff, and carries a 5-10% risk of infection or bleeding.
There’s another drug - vaptans - like tolvaptan. These block the hormone that makes your body hold water. Sounds perfect, right? But they cost $5,000-$7,000 per course and are limited to 30-day use. They’re not for everyone. Only used in very specific cases, and even then, they rarely replace paracentesis.

The Big Debate: Restrict or Not?
Here’s the real tension. On one side, you have decades of guidelines from AASLD and the European Association for the Study of the Liver (EASL) saying: cut sodium to 2 grams. On the other side, you have real-world data showing that moderate restriction (5-6.5 g salt) leads to better outcomes. Dr. Guadalupe Garcia-Tsao, who helped write the AASLD guidelines, says restriction still matters - but warns against pushing patients into malnutrition. Meanwhile, Dr. Pere Gines, whose team ran the 2022 trial, says strict restriction may actually harm some patients.
The middle ground? Many experts now say: don’t go too low. Aim for 2-3 grams of sodium per day - not zero. That’s about 5-6.5 grams of salt. It’s more realistic. It’s less likely to hurt your kidneys. And with proper diuretic therapy, it still works. The key is personalization. Someone with low sodium levels and swelling? Maybe they need tighter control. Someone with normal sodium and no kidney issues? Maybe they can afford a little more flexibility.
What You Can Do Right Now
- Track your sodium intake using a food diary app - focus on processed foods, not just salt.
- Ask your doctor for a sodium blood test before and after starting diuretics.
- Never take NSAIDs without checking with your liver specialist.
- Drink water only when thirsty. Don’t force fluids.
- If you’re losing weight faster than 1 kg/day, tell your doctor - you might be over-diuresed.
- Know the signs of infection: fever, belly pain, confusion. Ascites fluid can get infected - and that’s an emergency.
Ascites management isn’t about perfection. It’s about balance. Too much salt? Fluid builds up. Too little? Your kidneys fail. The goal isn’t to live on celery and water. It’s to live longer, with fewer hospital visits, and more control over your body. And that means listening - not just to guidelines, but to your own body, and your doctor.
Can I eat salt at all if I have ascites?
Yes, but you need to be careful. Most experts now recommend limiting sodium to 2-3 grams per day - not zero. That’s about 5-6.5 grams of table salt. Avoid processed foods, canned soups, and salty snacks. Cooking at home with fresh ingredients gives you the most control.
Why do I need to take two diuretics together?
Spironolactone and furosemide work in different parts of the kidney. Spironolactone blocks the hormone that makes you hold salt, while furosemide forces more salt out. Together, they’re more effective than either alone. The standard combo is 4 parts spironolactone to 1 part furosemide (like 100 mg and 25 mg). This balance helps avoid side effects like low potassium or dehydration.
How fast should I lose weight with ascites?
If you have swelling in your legs too, aim for up to 1 kg (2.2 pounds) per day. If you don’t have leg swelling, stick to 0.5 kg (1 pound) per day. Losing weight too fast can cause low blood pressure, kidney stress, or electrolyte imbalances. Your doctor will monitor your blood sodium and kidney function weekly until you’re stable.
Is ascites reversible?
In early stages, yes - with strict diet, diuretics, and stopping alcohol, some patients see their fluid go away completely. But once ascites appears, it usually means the liver is in advanced decline. Even if fluid clears, the underlying cirrhosis remains. The goal is to manage it long-term and prevent complications like infection or kidney failure.
What happens if I stop taking my diuretics?
Fluid will return - often quickly. Diuretics don’t cure the cause of ascites; they just manage the symptom. Stopping them without medical advice can lead to rapid fluid buildup, increased belly pressure, breathing trouble, or infection. Never stop or change doses without talking to your liver specialist.







13 Comments
I swear, if I see one more person say 'just cut salt' like it's easy... 😒 I have cirrhosis. My kid buys me bread because 'it's healthy'. It's got 400mg sodium PER SLICE. I can't even have a sandwich without crying. And don't get me started on restaurants. I used to love tacos. Now? I eat plain rice and stare at my food like it's a crime scene. They call it 'management'. I call it torture with a side of guilt.
The sodium dogma... it's a construct. A ritualized fear. We worship at the altar of guidelines as if they were scripture. But the body is not a lab rat. It is not a spreadsheet. The liver, in its broken state, does not obey the rules of physiology we learned in medical school. It rebels. It adapts. And when we force it into a 2g cage... it screams. It shuts down. The kidneys? They don't want to die. They want to survive. So they hoard. And we punish them for it. The real tragedy? We call it 'care'.
I've been managing ascites for 4 years. I started at 1.5g sodium. Ended up in the ER with hyponatremia. Now I'm at 3.5g. No hospital visits in 18 months. My numbers are stable. I cook everything. Read every label. But I let myself have a little cheese. A little olive oil. A little joy. The guidelines don't know your life. Your doctor should.
I just want to say 🙌 THANK YOU for writing this. My dad’s been on spironolactone for 2 years. We thought we were failing because he kept gaining weight. Turns out he was under-diuresed. Now he’s on the combo and losing 0.8kg/day. He’s eating pizza on Sundays. He’s smiling again. This isn’t just medicine. It’s dignity. 💙
You got this. Small wins count. One less processed snack. One homemade meal. One day without NSAIDs. That’s victory. You’re not behind. You’re not failing. You’re fighting. And that’s enough.
The 4:1 ratio of spironolactone to furosemide isn't arbitrary. It's pharmacokinetic synergy. Spironolactone blocks aldosterone in the distal tubule, while furosemide inhibits the NKCC2 cotransporter in the loop of Henle. Together, they hit multiple sodium reabsorption pathways. But here's the kicker: if you give too much furosemide, you trigger renin-angiotensin-aldosterone system rebound. That's why the ratio matters more than the absolute dose. Always monitor serum potassium and creatinine. And never, ever skip the albumin after paracentesis.
I read this whole thing and cried. Not because I'm sad. But because for the first time, someone didn't treat me like a broken machine. I've been told to eat celery for 3 years. I lost 15 pounds. I was malnourished. My liver didn't get better. My kidneys nearly quit. Then I found a doctor who said, 'Let's try 5g sodium.' I ate a sandwich. I cried. I felt human. Now I'm alive. Not just surviving. Living. Maybe the real cure isn't in the pill. Maybe it's in being heard.
You think this is about salt? No. It's about control. Pharma companies profit from diuretics. Hospitals profit from paracentesis. The 'guidelines' are written by people who get grants from drug companies. They want you scared. They want you dependent. They don't want you to know that fasting, intermittent fasting, and herbal detoxes can reverse ascites. But they'll never tell you that. Because it's not profitable. Read the studies. Look at the funding sources. The truth is buried. You're being manipulated.
In Nigeria, we say: 'The body is a river. You don't dam it-you guide it.' We don't starve the liver. We feed it wisdom. My uncle had ascites. We gave him bitter leaf tea. Coconut water. Fresh yam. No salt. No pills. He walked again. Maybe the answer isn't in the lab. Maybe it's in the soil.
Oh honey. You’re not 'failing' because you ate a bagel. You’re not a bad patient because you cried. You’re a person. And people eat bread. People want to taste food. This isn’t about perfection. It’s about showing up. Even if you messed up today. You’re still here. And that’s everything.
Stop overthinking. Salt restriction is outdated. Diuretics work. Period. If you’re losing weight at 1kg/day and your labs are clean, you’re doing fine. Stop reading Reddit. Stop Googling. Take your meds. Eat your food. Sleep. That’s the whole damn protocol.
I read this and laughed. 2g sodium? Please. I’m a chef. I’ve been cooking for 30 years. You think you can stop a cirrhotic liver from holding fluid by banning salt? Nah. It’s the sugar. It’s the carbs. It’s the damn beer. You’re blaming the salt because it’s easier than saying 'stop drinking' or 'stop eating processed crap'. The real villain? The American diet. Not the salt shaker.
The management of ascites necessitates a multidisciplinary approach grounded in evidence-based protocols. Sodium restriction remains paramount, with a target of 2g/day as per AASLD/EASL. Diuretic therapy must adhere to the 4:1 spironolactone-furosemide ratio to mitigate hypokalemia and maintain renal perfusion. Refractory cases require prompt paracentesis with albumin infusion at 8g/L of fluid removed. Non-compliance with NSAID avoidance significantly elevates hepatorenal syndrome risk. Adherence is non-negotiable.