Imagine spending your entire summer hiding under a t-shirt at the beach because your back is covered in strange, pale patches. You finally get them treated, the skin clears up, and then-just as the weather warms up again-they return. This cycle is incredibly common for people dealing with Tinea Versicolor is a common fungal skin infection caused by the overgrowth of yeast that naturally lives on everyone's skin. Also known as pityriasis versicolor, it isn't a sign of poor hygiene, nor is it contagious. Instead, it's a biological glitch where the yeast decides to move in and take over.
The real frustration isn't just the patches; it's the high chance of them returning. In fact, about 60-80% of people see the spots come back within a year. If you're tired of the "clear, then relapse" loop, you need a strategy that focuses on long-term management rather than just a quick fix. Here is how to handle the overgrowth and, more importantly, how to keep it from returning.
What Actually Causes the Patches?
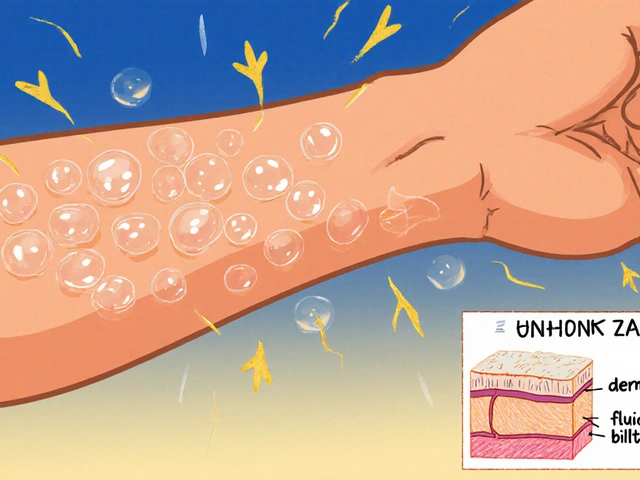
Your skin is home to a variety of organisms, including Malassezia, a genus of yeast. Usually, this yeast just hangs out in your oil glands without causing trouble. However, when conditions get just right-think high humidity, heavy sweating, or oily skin-the yeast overgrows. This overgrowth disrupts your skin's pigment.
Why the different colors? It depends on how the yeast interacts with your melanin. For some, the yeast produces azelaic acid, which actually blocks the pigment-producing cells. This creates those light or white patches. For others, the reaction causes inflammation, leading to pink, red, or brown spots. A frustrating reality is that sun exposure often makes these spots more obvious. While the rest of your skin tans, the affected patches stay pale, making them stand out like a sore thumb.
How Doctors Confirm the Diagnosis
Because these patches can look like vitiligo or eczema, getting a professional diagnosis is key. Dermatologists typically use a process called KOH microscopy. They scrape a tiny bit of skin and apply potassium hydroxide. Under a microscope, the yeast looks like "spaghetti and meatballs"-thin lines (hyphae) and round dots (budding yeast). This method is highly accurate and ensures you aren't using an antifungal on a condition that doesn't need one.
Clearing the Skin: Treatment Options
The goal of initial treatment is to kill off the excess yeast and allow the skin to recover. Depending on how widespread the infection is, you'll likely encounter two main paths:
- Topical Treatments: For mild to moderate cases, a Selenium Sulfide shampoo (like Selsun Blue) is often a first choice. You don't just wash with it; you apply it to the skin and let it sit for about 10 minutes daily for two weeks.
- Oral Medications: If the infection covers a large part of your body, a doctor might prescribe Fluconazole. This is a powerful antifungal pill taken weekly for a few weeks. Because it's systemic, doctors may monitor your liver function to ensure everything is running smoothly.
| Treatment Method | Typical Agent | Best For... | Pros/Cons |
|---|---|---|---|
| Topical Shampoo | Selenium Sulfide / Ketoconazole | Localized patches | Easy to apply, low side effects; can be messy. |
| Topical Cream | Clotrimazole / Terbinafine | Small, concentrated areas | Fast acting; tedious for large body areas. |
| Oral Medication | Fluconazole | Widespread or resistant cases | Highest clearance rate; requires prescription and monitoring. |
The Secret to Preventing Recurrence
Getting the spots to disappear is the easy part; keeping them gone is the challenge. Since Malassezia never fully leaves your skin, it's always waiting for the right moment to grow back. This is why "maintenance therapy" is non-negotiable for people who get frequent flare-ups.
The most effective strategy is using a Ketoconazole 2% shampoo as a preventative wash once a month. Think of it like a "reset button" for your skin's yeast levels. By applying this monthly, you keep the population in check before it reaches the threshold where it causes visible patches. If you live in a hot, humid climate, you might need to do this more frequently during the summer months.
Beyond the medication, your daily habits play a huge role. Since this yeast loves oil, avoiding heavy, oil-based lotions and skincare products on your chest and back can starve the fungus. Switching to moisture-wicking fabrics-like the ones used in athletic gear-helps keep your skin dry and reduces the humidity that the yeast craves.
Common Pitfalls and Mistakes
One of the biggest mistakes people make is scrubbing their skin raw. There is a common myth that this is caused by being "dirty," leading some to use harsh exfoliants. In reality, excessive scrubbing can damage your skin barrier, making it easier for the yeast to penetrate and thrive. Be gentle; the goal is to manage the fungus, not strip your skin.
Another point of frustration is the "ghost patches." Even after the fungus is dead, the light spots can remain for six months or more. This isn't because the treatment failed; it's simply because your skin needs time to produce melanin again and catch up to the rest of your tan. Don't panic and restart intensive medication if the spots are still there but not spreading-just give it time.

Who is Most at Risk?
While anyone can get it, a few factors make you a prime target for recurrences. Adolescents and young adults are hit hardest because of the surge in sebum (oil) production during those years. Additionally, if your immune system is compromised-whether due to chronic steroid use, diabetes, or other health conditions-your body has a harder time keeping the yeast in check.
Geography also matters. If you're in a tropical region with 70-90% humidity, your risk of recurrence jumps significantly compared to someone in a temperate zone. If you're traveling to a humid climate, it might be a good idea to start your preventative wash routine a few weeks before you leave.
Is Tinea Versicolor contagious?
No, it is not. The yeast that causes the infection is already present on most people's skin. The condition happens when that yeast overgrows, not because you "caught" it from someone else.
Why do the patches stay white even after treatment?
The yeast produces an acid that stops your skin from tanning. Even after the yeast is gone, it takes time for the pigment-producing cells to recover. These patches usually fade naturally over several months as you spend time in the sun.
Can I use over-the-counter creams?
Yes, many antifungal creams like clotrimazole work well for small areas. However, for larger areas like the back or chest, medicated shampoos are often more practical and effective.
Does diet affect Tinea Versicolor?
There is no strong clinical evidence that specific foods cause the overgrowth. The primary triggers are environmental (heat, humidity) and biological (oil production and immune health).
How often should I do maintenance washes?
For most people, a monthly wash with ketoconazole shampoo is enough to prevent recurrence. If you have very oily skin or live in a tropical climate, your doctor might suggest every two weeks during the summer.
Next Steps for Long-Term Success
If you've just finished your first round of treatment, don't just stop. Set a recurring reminder on your phone for your monthly maintenance wash. This simple habit is the difference between a clear summer and a repeat visit to the dermatologist.
If you notice the patches returning despite your efforts, it's worth chatting with your doctor about "antifungal resistance." While rare, some strains of yeast can become less sensitive to common treatments, and you might need a different active ingredient to get things back under control. Stick to breathable fabrics, keep the oil under control, and stay consistent with your preventative routine.






14 Comments
I've seen a lot of people get better results by rotating between two different antifungal shampoos so the yeast doesn't get used to one ingredient
helpful guide keep it simple
It is so frustrating when you think you're finally clear and then those spots reappear out of nowhere. Just remember to be patient with the ghost patches since they really do take a long time to fade
Oh wow, look at us just trusting big pharma's "maintenance therapy" blindly. I'm sure the pharmaceutical companies are just thrilled we're all setting recurring calendar alerts to buy their overpriced shampoo every single month for the rest of our lives. Truly a masterpiece of a business model
Typical. They push these chemical concoctions while ignoring the fact that these "biological glitches" are likely just the body reacting to the toxins they're pumping into our water supply. I've read that certain frequencies can actually disrupt fungal growth, but of course, a standard medical guide would never mention that because it doesn't make a profit for the elite few controlling the narrative
Shampoos are too basic. Try oil-free diets
The lack of mention regarding the impact of laundry detergents on skin barrier permeability is... staggering!!! One simply cannot ignore the synergy between synthetic fragrances and fungal proliferation!!!!
Yall really need to focus on your inner energy and gut health. Most of these skin issues are just manifests of a blocked chakra and bad vibs. Stop relyin on chemicals and start meditateing
Let's get after it everyone! Consistency is the only way to win this fight against the yeast! I actually started using a small exfoliating brush but very gently as mentioned here and it's a total game changer for the texture of the skin! You guys have to stay disciplined with those monthly washes or you're just wasting your time! Let's crush these patches together!
This is just Western medicine talking 🙄 My grandmother used natural neem leaves and it worked way better than some fancy shampoo from a lab! Stop following these foreign guides and trust traditional wisdom 🇮🇳💪
The phrasing in this guide is remarkably pedestrian and the advice is utterly derivative. It is quite exhausting to encounter such banal suggestions in an era where we should be discussing the systemic failures of dermatological research
This whole thing reeks of a coordinated effort to make us dependent on antifungal agents. It's a total scam to keep us in a loop of "maintenance" while the real cause is likely something the government is hiding about atmospheric humidity levels. Totally bogus advice for the sheeple
I strongly insist that every single person suffering from this condition adheres strictly to the professional medical guidelines provided here! There is absolutely no excuse for neglecting your skin health when the solution is so readily available!
It's interesting to see how different cultures approach this, but a balanced approach combining the mentioned medical treatments and gentle home care usually works best for everyone