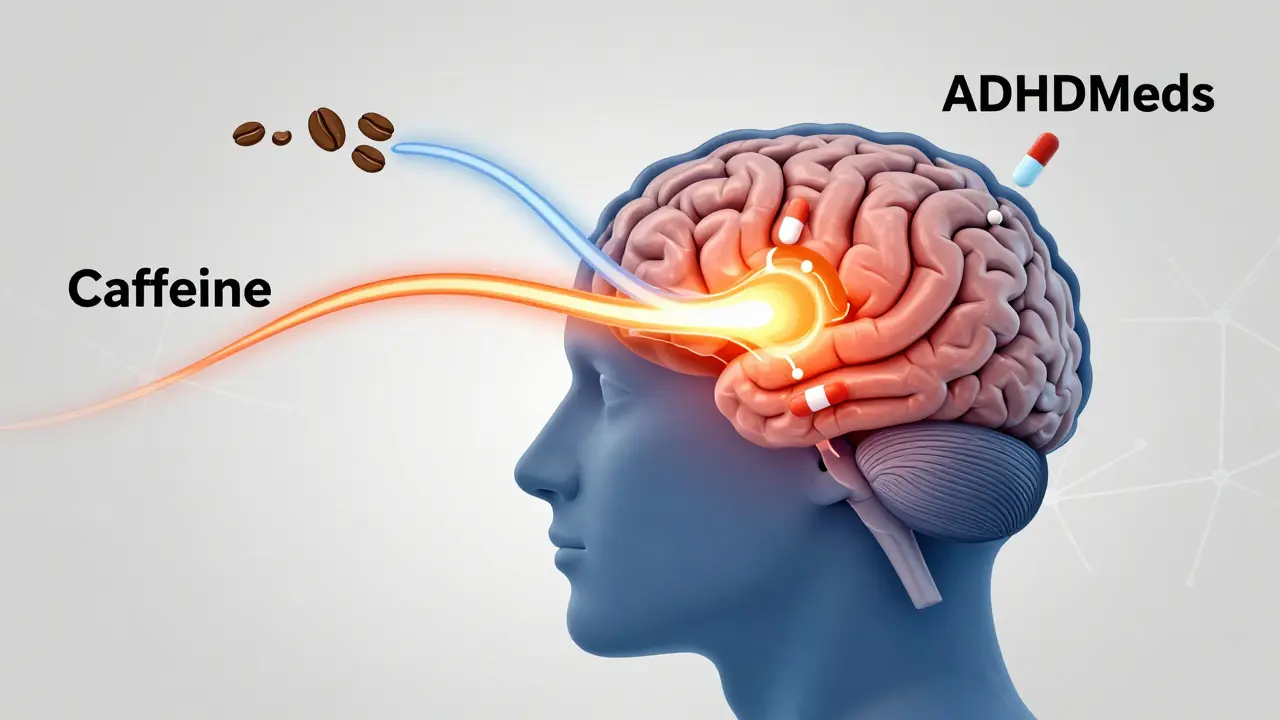
Do you grab a cup of coffee every morning to help your ADHD medication kick in? You are not alone. Millions of people with attention deficit hyperactivity disorder (ADHD) combine their prescription stimulants with caffeine, hoping for better focus or a smoother start to the day. But mixing these two powerful central nervous system (CNS) stimulants is like pouring gasoline on a fire that’s already burning. It can make the flames burn hotter and brighter, but it also increases the risk of an explosion.
This interaction between caffeine, chemically known as trimethylxanthine, and prescription drugs like Adderall (which contains amphetamine and dextroamphetamine) is complex. While some users report enhanced productivity, others experience severe anxiety, heart palpitations, and crashes that ruin their afternoon. Understanding how these substances interact in your body is crucial for staying safe and getting the most out of your treatment plan.
How Caffeine and Stimulants Work Together
To understand the risk, we need to look at what happens in your brain. Both caffeine and ADHD medications target dopamine, a neurotransmitter responsible for reward, motivation, and focus. People with ADHD often have lower baseline levels of dopamine or inefficient dopamine receptors. Prescription stimulants work by blocking the reuptake of dopamine and norepinephrine, keeping them active in the brain longer. This leads to improved concentration and reduced impulsivity.
Caffeine works differently but achieves a similar end result. It blocks adenosine receptors, which prevents you from feeling tired, and indirectly boosts dopamine release. When you take both, you are hitting the same pathways from different angles. This creates a synergistic effect. In pharmacology, synergy means the combined effect is greater than the sum of the individual effects. For some, this means laser-like focus. For others, it means overstimulation.
A 2016 meta-analysis published in the Journal of the American Academy of Child & Adolescent Psychiatry found that prescription stimulants are approximately three to five times more effective than caffeine alone for managing core ADHD symptoms. However, adding caffeine to a potent drug like Adderall doesn't necessarily triple the benefits; it often triples the side effects.
The Hidden Dangers: Cardiovascular Risks
The most significant concern with combining caffeine and ADHD meds is the strain on your cardiovascular system. Both substances increase heart rate and blood pressure. When taken together, they can cause tachycardia (rapid heartbeat) and hypertension (high blood pressure) much more easily than either substance alone.
Dr. David Goodman, an Assistant Professor at Johns Hopkins University School of Medicine, warned in a 2022 publication in Current Psychiatry Reports that combining two CNS stimulants without medical supervision increases the risk of tachycardia by 37% and hypertension by 29%. These statistics come from data collected at VA Hospitals in 2021. For individuals who already have underlying heart conditions, this combination can be dangerous. According to a 2023 study in JAMA Internal Medicine, 23% of adult ADHD patients have comorbid cardiovascular issues, making this group particularly vulnerable.
The American Heart Association recommends no more than 200 mg of caffeine daily for individuals with cardiac conditions. The FDA defines the maximum safe caffeine intake for healthy adults as 400 mg per day, roughly equivalent to four 8-ounce cups of brewed coffee. However, "safe" limits assume you are not taking other stimulants. If you are on Adderall, even 100 mg of caffeine might push your system too far.
Anxiety, Jitters, and the Crash
Beyond heart health, the mental side effects are where many users struggle. Anxiety is the most common complaint. A survey conducted by the National Alliance on Mental Illness (NAMI) in 2022 found that 33% of adult ADHD patients who combined caffeine and stimulants required medical attention for side effects, compared to only 8% of those using medication alone.
User experiences online reflect this tension. On Reddit’s r/ADHD community, a July 2023 thread with 1,247 comments showed that while 62% of respondents used caffeine with their medication, 59% experienced increased anxiety. One user, u/ConcentratedChaos, noted: "Taking my 20mg Adderall with one cup of coffee (95mg caffeine) makes me feel amazing until hour 3, then I crash hard with severe anxiety."
This "crash" happens because caffeine has a shorter half-life than most ADHD medications. Caffeine’s half-life ranges from 3 to 7 hours, averaging 5 hours according to a 2022 study in the Journal of Clinical Pharmacology. Adderall, however, has a half-life of 10 to 13 hours. As the caffeine wears off, its calming or focusing effects disappear, but the medication is still circulating in your system. This imbalance can lead to irritability, mood swings, and fatigue later in the day.
Timing and Dosing Strategies for Safety
If you choose to use both, timing is everything. The goal is to avoid peak concentrations of both substances overlapping in your bloodstream. Granite Mountain Behavioral Health Center’s 2023 clinical guidelines recommend waiting at least 4 to 5 hours between caffeine consumption and ADHD medication. Their data from 1,200 patients showed that spacing doses reduced side effects by 68% while maintaining cognitive benefits.
Here is a practical approach to managing this combination:
- Start Low: Begin with no more than 100 mg of caffeine (one small coffee) while on stimulants. Board-certified psychiatrist Dr. Ned Hallowell suggests this limit based on his 2022 clinical data, noting that 31% of initial combination users experience anxiety or heart palpitations.
- Space It Out: Do not drink coffee at the exact same time you take your medication. If you take your med in the morning, wait until mid-afternoon for your coffee, or vice versa. Avoid caffeine within 4-5 hours of bedtime to prevent sleep disruption.
- Eat Food: Taking both substances with food reduces gastrointestinal distress. A 2021 study in the Journal of Psychopharmacology found that 45% of combination users experienced stomach issues, which were significantly reduced when meals were involved.
- Monitor Your Body: Use a wearable device to track your heart rate. If you notice sustained elevations above your normal resting rate, cut back on caffeine immediately.
The Role of L-Theanine
Some researchers are looking at ways to mitigate the jitters caused by this combination. L-theanine, an amino acid found in tea, has shown promise. A 2020 study by Kahathuduwa et al., involving boys diagnosed with ADHD, demonstrated that while caffeine alone worsened inhibitory control, the combination of L-theanine and caffeine improved total cognition composite scores.
L-theanine decreases GABA levels and increases glutamate modulation, creating a calming effect that may counteract the anxiety induced by caffeine and stimulants. The NIH-funded research suggests a ratio of 3:1 (L-theanine to caffeine) might be optimal. Preliminary data from 127 participants indicated this ratio reduced mind-wandering and task-related reactivity in the default mode network of the brain. However, this is still emerging science, and you should consult your doctor before adding supplements to your regimen.

Who Should Avoid This Combination?
Not everyone can safely mix caffeine and ADHD meds. Certain groups face higher risks and should likely avoid caffeine entirely while on stimulants:
- Children and Adolescents: The American Academy of Pediatrics specifically cautions against combining caffeine with prescription stimulants for young patients due to developing cardiovascular systems and unpredictable metabolism.
- Slow Metabolizers: Genetics play a huge role. About 40% of the population are "slow metabolizers" of caffeine due to variations in the CYP1A2 gene, according to a 2022 study in the Pharmacogenomics Journal. These individuals process caffeine slowly, leading to higher accumulation in the blood and increased side effects.
- People with Anxiety Disorders: If you have comorbid anxiety, the stimulating effects of caffeine can exacerbate panic attacks and general worry.
- Pregnant Women: High caffeine intake during pregnancy is linked to various complications. Combining it with stimulants adds another layer of uncertainty that most doctors advise avoiding.
Practical Checklist for Daily Management
Managing this interaction requires discipline. Here is a simple checklist to keep your routine safe and effective:
| Action | Why It Matters | Target Goal |
|---|---|---|
| Track Intake | Hidden sources add up | < 200mg total caffeine/day |
| Check Heart Rate | Detects overstimulation | Resting HR < 100 bpm |
| Space Doses | Reduces peak overlap | 4-5 hour gap between substances |
| Eat Before Taking | Prevents GI distress | Full meal or snack beforehand |
| Hydrate | Counters dehydration from stimulants | 2-3 liters of water daily |
Remember, the learning curve for managing this combination typically takes 2 to 4 weeks. During this time, track your caffeine intake, including hidden sources like chocolate, energy drinks, and certain pain relievers. Use standardized scales like the ASRS-v1.1 to monitor symptom severity. If you find yourself needing more caffeine to get the same effect, or if your anxiety is increasing, it is time to step back and talk to your healthcare provider.
Can I drink coffee with my Adderall?
Yes, but with caution. Many people do, but it increases the risk of side effects like anxiety, jitteriness, and high blood pressure. It is best to space them out by 4-5 hours and limit caffeine to under 200mg per day. Always consult your doctor first, especially if you have heart issues.
Does caffeine make ADHD medication less effective?
No, caffeine does not make ADHD medication less effective. In fact, it may temporarily enhance focus for some users. However, it can worsen side effects and lead to a harder "crash" later in the day because caffeine wears off faster than most prescription stimulants.
What are the signs of too much caffeine with ADHD meds?
Signs include rapid heartbeat (tachycardia), high blood pressure, severe anxiety, panic attacks, insomnia, tremors, and gastrointestinal distress. If you experience chest pain or difficulty breathing, seek medical attention immediately.
Is it safer to take caffeine or ADHD meds alone?
Taking ADHD medication alone is generally safer for treating ADHD symptoms. Caffeine alone is 60-70% less effective for core ADHD symptoms than prescription stimulants. Combining them increases health risks without providing proportional therapeutic benefits for most people.
How long does caffeine stay in your system with ADHD meds?
Caffeine has a half-life of 3-7 hours, meaning it takes about 5 hours for half of it to leave your body. ADHD medications like Adderall last much longer, with a half-life of 10-13 hours. This mismatch can cause side effects as the caffeine wears off while the medication is still active.
Can L-theanine help reduce caffeine jitters?
Research suggests L-theanine may help. Studies indicate that combining L-theanine with caffeine can improve cognition and reduce anxiety associated with stimulants. A 3:1 ratio of L-theanine to caffeine appears promising, but you should discuss this with your doctor before trying it.
Are slow caffeine metabolizers at higher risk?
Yes. About 40% of people are slow metabolizers due to genetic factors (CYP1A2 gene). These individuals process caffeine more slowly, leading to higher levels in the blood and a greater risk of adverse effects when combined with ADHD medications.
Should children avoid caffeine with ADHD meds?
The American Academy of Pediatrics advises against combining caffeine with prescription stimulants for children and adolescents. Their developing bodies and brains are more susceptible to cardiovascular risks and behavioral side effects.