Medication Safety & Formulation Checker
Your Profile
Safety Assessment
Click "Generate Safety Report" to see your results.
The Hidden Differences Between Your Meds
It's easy to assume that all pills work the same way until they don't. One day you're fine, and the next, a new bottle of your usual blood pressure med leaves you feeling dizzy. Or maybe you switch to a "natural" herbal remedy for sleep, only to find your regular antidepressant stops working properly. Medication Classesare groups of drugs categorized by how they affect the body and treat conditions. Understanding which class you're taking is crucial because distinct categories carry different risks. From prescription drugs to over-the-counter supplements, the rules governing safety aren't uniform. What looks safe on the label might interact dangerously with other treatments you're already taking. Knowing the specifics helps you avoid unwanted reactions and ensures your treatment plan actually works.
Regulatory Gaps: Why Prescriptions Differ from Supplements
The biggest factor in side effect profiles isn't just the chemical itself; it's who checks it. In the United States, the U.S. Food and Drug Administration (FDA)is the government agency responsible for protecting public health through the regulation of food, drugs, and medical devices manages prescription and over-the-counter medications with rigorous clinical trials. These drugs must prove safety and efficacy before hitting the shelves. However, complementary medicines-like vitamins, minerals, and herbals-operate under a different legal framework known as the Dietary Supplement Health and Education Act (DSHEA)federal law that regulates labeling and manufacturing of dietary supplements in the US passed in 1994. Under this act, pre-market approval isn't required.
This creates a significant safety disparity. A study referenced by University Hospitals (2022) highlights that while conventional medicine faces strict oversight, supplements can cause side effects, interactions, and even poisoning without the same level of scrutiny. For instance, EchinaceaPurples Conefloweran herbal supplement often used to boost immunity, has been linked to over 20 different types of adverse reactions, ranging from mild skin rashes to serious asthma attacks. If you are allergic to plants in the ragweed family, Echinacea could trigger a severe reaction without warning labels found on prescription bottles.
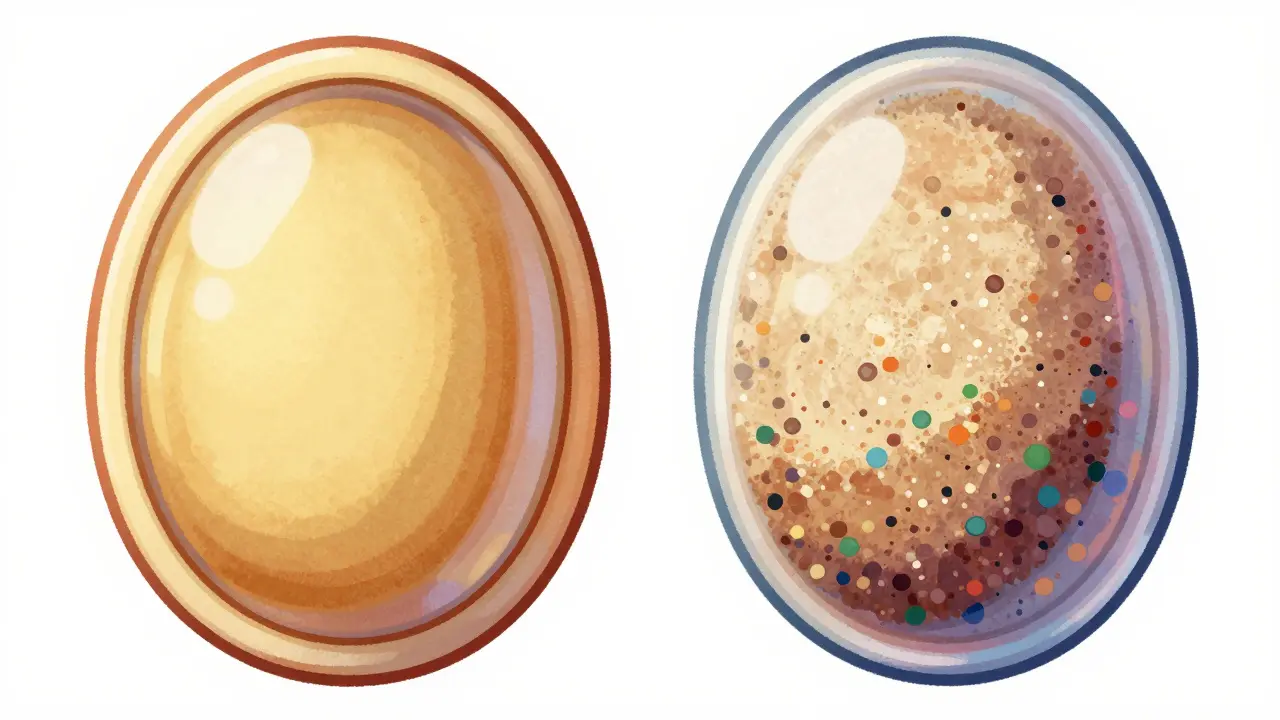
Brand-Name Versus Generic: Is the Switch Worth the Risk?
Many patients worry when their doctor switches them to a cheaper version of their medicine. The core issue here lies in bioavailability. Federal mandates require generic drugs to contain the same active ingredients as brand-name versions and show bioequivalence within an 80% to 125% absorption range. Research indicates an average difference of roughly 3.5% in absorption between the two, generally considered clinically acceptable. However, the inactive ingredients-fillers, binders, and dyes-often differ.
| Feature | Brand-Name Drug | Generic Drug |
|---|---|---|
| Active Ingredient | Mandatory Same Composition | Mandatory Same Composition |
| Precision Manufacturing Standards | Bioequivalence Range: 80-125% | |
| Inactive Ingredients | Consistent per Manufacturer | Varies by Manufacturer |
| Standardized Fillers/Dyes | Lactose, Gluten, Dyes May Vary | |
| Cost Factor | Higher Price Point | Significantly Lower Cost |
For most people, these differences don't matter. But if you have lactose intolerance, a generic pill filled with dairy products might cause stomach distress that the brand-name version didn't. Conversely, someone sensitive to a specific dye in a brand drug might find relief in a generic. Dr. Howell from Pullman Regional Hospital advises checking ingredient lists specifically for allergens like soya lecithin, benzoates, or sulfites when switching formulations.
The Narrow Therapeutic Index Warning
There is one critical exception where the "generic vs. brand" debate becomes life-altering: Narrow Therapeutic Index (NTI) Drugsmedications where small changes in dosage can lead to toxic effects or lack of efficacy. For these drugs, even slight variations in blood concentration can be dangerous. Examples include LevothyroxineSynthroida synthetic form of thyroid hormone used to treat hypothyroidism (used for thyroid issues) and WarfarinCoumadinan anticoagulant medication used to prevent blood clots (a blood thinner).
A study published in PMC noted that patients switching between manufacturers for anti-seizure meds (antiepileptics) sometimes experienced more side effects and increased costs from doctor visits. While general cardiovascular data suggests equivalence, individual physiology can react unpredictably to minor shifts in release rates or absorption. For NTI drugs, University Hospitals pharmacists recommend staying with one manufacturer to minimize variability. You shouldn't flip-flop between generic batches for these specific treatments without monitoring your blood levels closely.

Natural Doesn't Mean Safe: Herbal Interactions
A dangerous assumption persists that "natural equals safe." Medical News Today (2023) emphasizes that natural medicines can cause side effects just as severe as pharmaceutical ones. The real risk often comes from interactions rather than the single ingredient alone. Consider St. John's Wortan herbal supplement commonly used to treat depression and anxiety. It works by increasing serotonin levels. If you take this alongside prescription antidepressants, you risk serotonin toxicity. Symptoms include high temperature, tremors, and low blood pressure, requiring emergency care.
Bleeding risks are another silent threat. Herbs like Feverfewa plant extract used traditionally for migraines, Ginkgo, and Chamomile increase bleeding tendencies. Combining these with blood thinners like warfarin or aspirin magnifies the risk of hemorrhage. Even pregnancy poses specific dangers; animal experiments suggest Feverfew can trigger uterine contractions, leading to miscarriage. These interactions highlight why transparency between your doctors and pharmacists is non-negotiable.
Monitoring Your Medication Safety
You need to take charge of your regimen when prescriptions change. Start by requesting your pharmacist to list the manufacturer of any generic you fill, especially for heart or thyroid medications. Check the patient information leaflet for inactive ingredients if you have known allergies (lactose, gluten, soy). Finally, maintain a logbook of your symptoms when starting any new therapy. It is difficult to distinguish whether a rash is a side effect or a symptom of your illness, as noted by the Better Health Channel (2023). Tracking timing helps your doctor determine causality.
Steps to Ensure Medication Consistency
- Keep Records: Write down the name of the pharmacy and the specific manufacturer code of your generic drug if you feel symptoms changing.
- Check Labels: Scan the "inactive ingredients" list for known allergens like dyes or preservatives.
- Avoid Mixing Alcohol: Alcohol interacts with antibiotics and other meds, causing flushing or digestive upset hours after drinking.
- Ask About NTI Status: Confirm with your doctor if your drug falls into the narrow therapeutic category requiring strict consistency.
- Disclose Supplements: Always tell your doctor about every vitamin or herbal tea you consume regularly.









13 Comments
The regulatory oversight disparity between pharmaceutical compounds and dietary supplements remains truly egregious. One might perceive natural remedies as benign placeholders when toxicology dictates otherwise entirely. Clinical trials establish efficacy thresholds that herbal blends completely bypass during manufacturing. Bioavailability metrics shift wildly across different excipient formulations within generic counterparts.
Patients often suffer due to inconsistent absorption rates hidden behind standard labeling protocols. Lactose fillers represent merely one facet of allergenic contamination found in cheaper pill presses. Dye sensitivities can trigger dermal reactions that manifest hours after ingestion occurs silently. Therapeutic indices narrow significantly when switching manufacturers without active serum concentration tracking.
Warfarin dosages require absolute precision which fluctuates unpredictably with batch variations constantly. Serotonin syndrome emerges rapidly when combining St Johns Wort with prescribed monoamine oxidase inhibitors. Emergency departments overflow with preventable cases linked to undisclosed supplement usage histories. Transparency within patient portals regarding inactive ingredients remains woefully inadequate in practice today.
Physicians rarely screen for herb drug interactions unless explicitly prompted by patient disclosure voluntarily. Safety profiles demand rigorous documentation beyond mere packaging claims made by unregulated entities. Understanding pharmacological classifications prevents unnecessary hospital visits stemming from avoidable confusion.
the system protects big profits not human lives through lax supplement laws
its scary how much we dont know about what goes into our bodies honestly teh regulation gaps are real i wish i knew more before taking anything new because mistakes happen and nobody likes feeling sick for no reason
Pharmacokinetic variability is a major concern for patients on chronic therapy regimens. Bioequivalence limits allow fluctuations that may impact clinical outcomes for sensitive subpopulations. Serum concentration monitoring becomes essential when therapeutic windows are narrow. We must prioritize patient education regarding inert ingredient disclosures. Consistency in formulation supports predictable metabolic processing pathways effectively.
Strict adherence to safety protocols is mandatory for everyone regardless of cost savings offered by generics. Deviating from established therapeutic guidelines introduces unnecessary liability and health risks. Compliance with manufacturer specifications ensures optimal drug delivery mechanisms function correctly. Ignoring formulation differences undermines treatment integrity entirely.
i get the concern but we cant live in fear :) sometimes the risk is worth the savings for most folks depending on what med it is
totally agree with you on that note
people really need to stop trusting everything they see on tv 🛑🚫💊 natural does not mean safe i swear people are so gullible 😤😠
its amazing how much responsibility we hold for keeping track of our own meds honestly doctors are busy and might forget to ask about the vitamins you take daily supplements interact with prescriptions in ways that nobody tells us upfront about clearly generic brands save money but sometimes the fillers cause stomach issues unexpectedly we should check the label for gluten or lactose if we have allergies already known thyroid meds need the same maker to work consistently for your body chemistry bleeding risks increase when you add ginger or ginkgo to your blood thinner routine pregnancy changes how drugs metabolize so extra caution is needed there definitely tracking symptoms in a journal helps doctors spot patterns faster than memory alone alcohol flushes can ruin antibiotic treatment effectiveness if consumed too close together asking the pharmacist for manufacturer codes builds a better record for future switches consistency is key when managing chronic conditions over long periods of time slowly staying informed empowers you to make better choices about your health overall small adjustments in routine can prevent big problems down the road eventually trust yourself to notice changes and speak up whenever something feels off really
This information is incredibly useful!!! Everyone needs to read this!!! It could literally save lives!!!!! We have to pay attention to labels!!!
sticking to one manufacturer reduces variance significantly for thyroid patients especially those on levothyroxine or warfarin where margins are thin and errors costly
important info here we should respect boundaries around health decisions :) thanks for sharing
Taking charge of medication management requires diligence but yields significant health benefits ultimately. Records of pharmacy locations help isolate variables when adverse events surface unexpectedly. Inactive ingredient lists provide crucial data points for individuals with specific dietary restrictions. Avoiding alcohol consumption near dosing times mitigates unpleasant physiological reactions effectively.
Narrow therapeutic index drugs warrant specific conversations regarding manufacturer stability requirements. Full disclosure of supplements ensures comprehensive care plans reflect total intake accurately. Medical teams appreciate proactive patients who maintain logs of symptom onset timings precisely. Knowledge acts as the primary defense against unforeseen complications arising from polypharmacy scenarios. Generic bioequivalence ranges allow slight deviations that accumulate over extended usage periods. Herbal interactions amplify bleeding risks significantly when combined with anticoagulant medications regularly.
Serotonin toxicity presents a severe danger when antidepressants meet mood enhancing botanical agents. Manufacturer consistency minimizes fluctuation levels within critical hormonal replacement therapies. Patient advocacy groups highlight these disparities to push for stricter labeling enforcement policies soon. Education bridges the gap between regulatory frameworks and practical daily medication administration safely. Prioritizing safety checks transforms potential emergencies into manageable preventative maintenance tasks easily.